Cervical Myelopathy
Spinal Cord Compression in the Neck
Quick Summary
Cervical myelopathy occurs when the spinal cord in the neck is compressed, most often due to spinal stenosis or arthritis.
Common cause of balance problems and hand clumsiness
Symptoms often develop slowly and progressively
MRI is the best test to confirm spinal cord compression
Surgery is commonly recommended to prevent worsening
Early diagnosis improves outcomes
-
Myelopathy means dysfunction of the spinal cord.
-
A pinched nerve affects one nerve, while myelopathy affects the spinal cord.
-
Yes. Because the spinal cord controls the arms and legs, symptoms can be widespread.
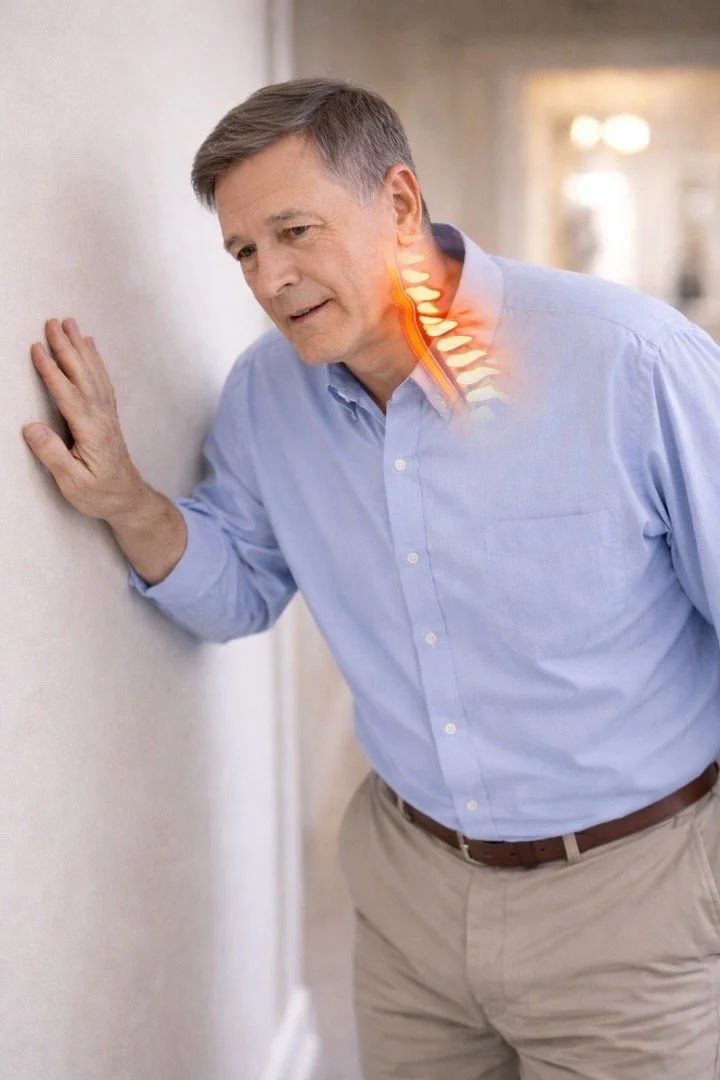
What is cervical myelopathy?
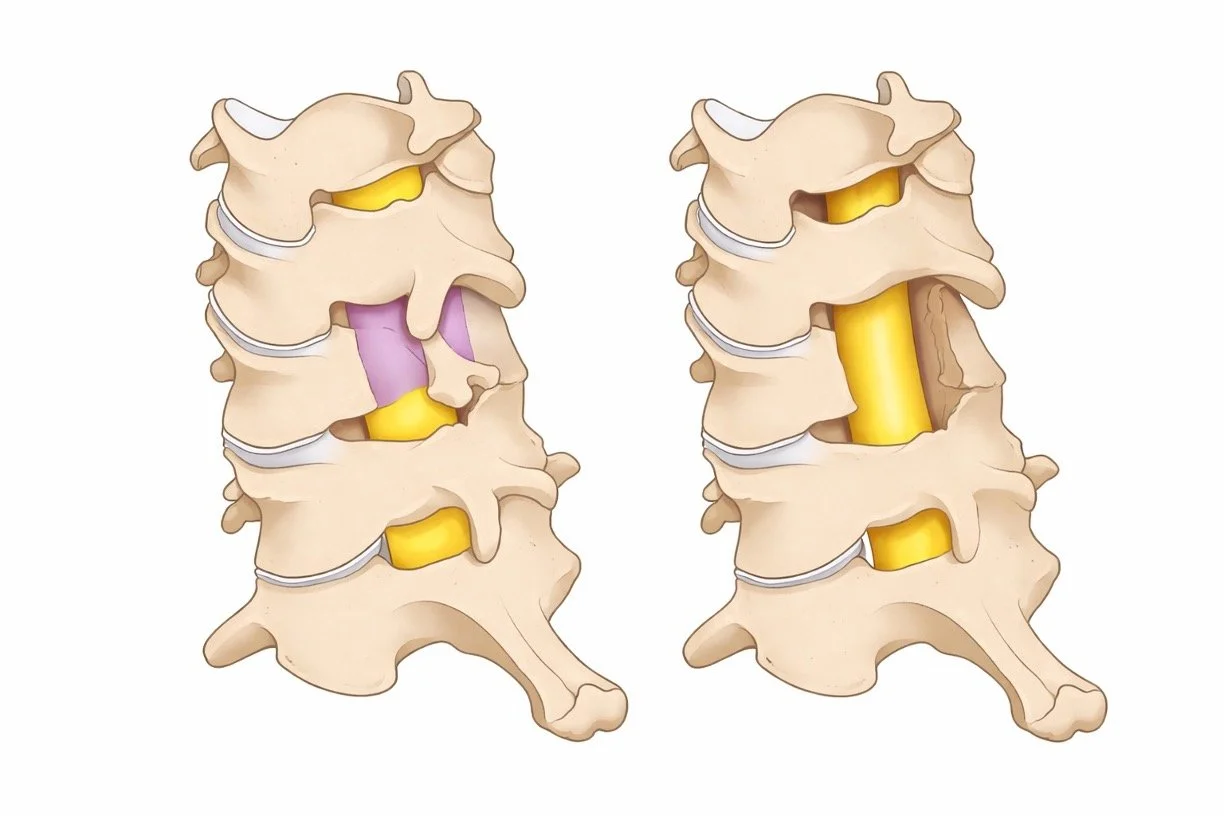
Cervical myelopathy means that the spinal cord in the neck is being compressed.
The spinal cord carries signals from the brain to the arms and legs. When it is compressed, these signals do not travel normally, leading to problems with balance, coordination, and strength.
What are the symptoms of cervical myelopathy?
Symptoms often involve both the arms and legs and may include:
Difficulty with balance or walking
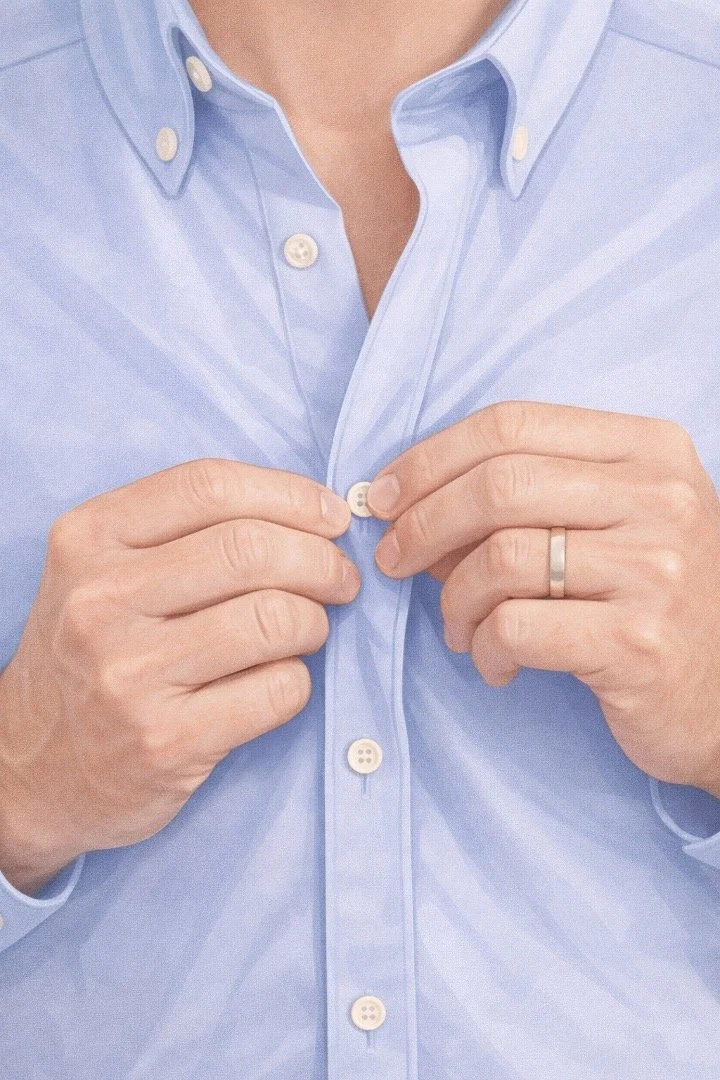
Hand clumsiness or dropping objects
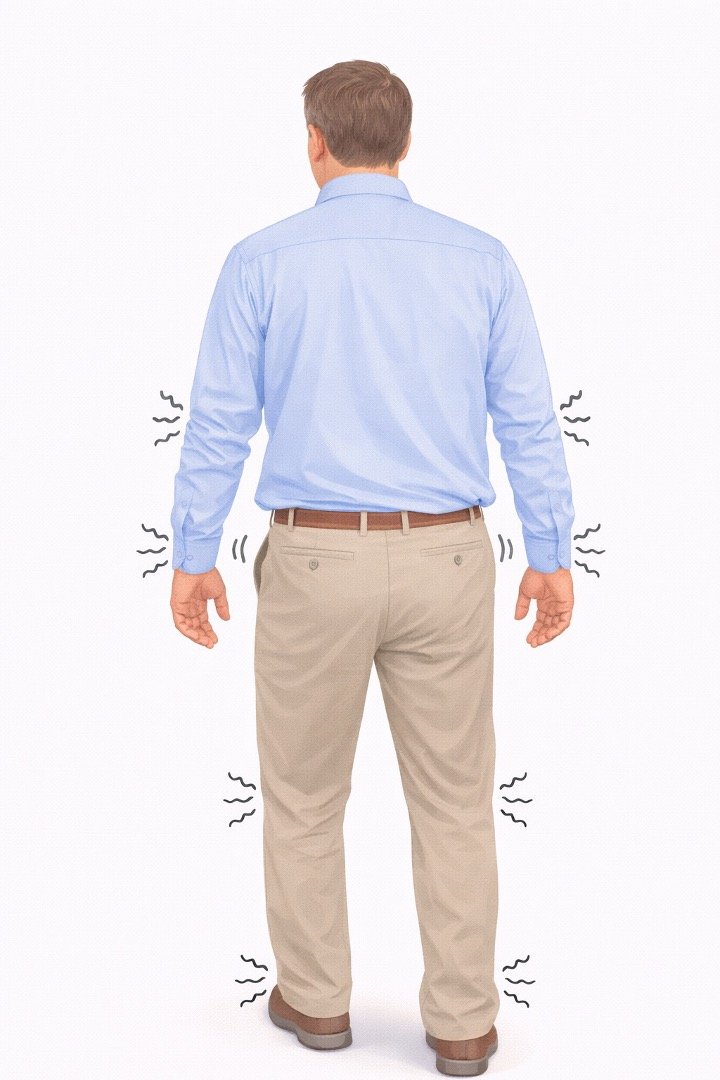
Weakness or stiffness in the legs
Numbness or tingling in the hands
Neck pain or stiffness (may be mild)
-
Spinal cord compression affects fine motor control.
-
Signals from the brain to the legs are disrupted.
-
Yes. Early symptoms are often mild and easy to overlook.
-
Progressive weakness, loss of coordination, or balance problems should be evaluated promptly.
What causes cervical myelopathy?
The most common cause is cervical spinal stenosis, usually from age-related changes.
Other causes include:
Arthritis and bone spurs
Disc bulging or herniation
Thickened spinal ligaments
Congenitally narrow spinal canal
-
Usually no. Symptoms often develop gradually over time.
-
Yes, especially if it presses directly on the spinal cord.
-
It can be, but most cases are degenerative.
How is cervical myelopathy diagnosed?
Diagnosis includes:
Detailed medical history
Neurological examination
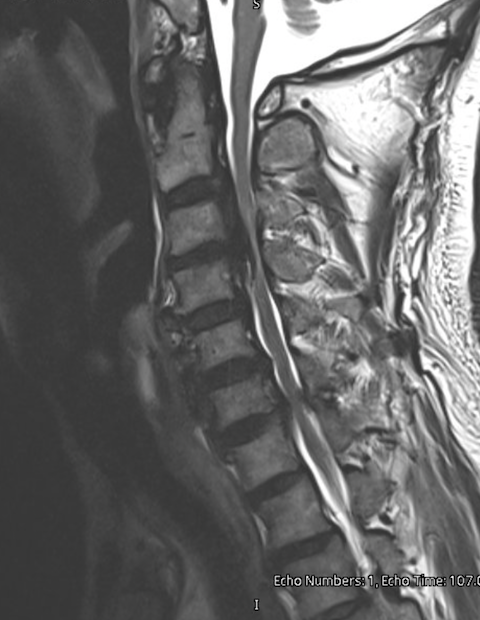
MRI of the cervical spine
MRI shows spinal cord compression and can reveal signal changes within the cord.
-
MRI shows the spinal cord directly.
-
It suggests stress or injury to the spinal cord.
-
X-rays or CT scans may help evaluate bone structure.
-
They are different tests. MRIs show your spinal cord and nerves. XR shows your spine alignment. Having both are helpful for your physician.
Do I need surgery for cervical myelopathy?
Surgery is commonly recommended for cervical myelopathy.
Non-surgical treatments do not reliably stop progression of spinal cord damage
Surgery is considered when:
Myelopathy is diagnosed on exam and imaging
Symptoms are worsening
Balance or hand function is affected
-
Because spinal cord damage can worsen and may not recover without decompression.
-
It can be time-sensitive, especially if symptoms are progressing.
-
Symptoms may stabilize, but typically they are more likely to get worse over time, rather than better.
What types of surgery treat cervical myelopathy
Surgery focuses on relieving pressure on the spinal cord and may include:
The approach depends on spinal alignment, number of levels involved, and location of compression.
-
The approach depends on where compression is located.
-
Yes. The main goal is to prevent further damage.
-
Improvement varies and depends on severity and timing.

When should I see a spine specialist?
You should seek evaluation if you have:
Neck or arm pain persists despite treatment
You develop weakness, numbness, or coordination problems
Symptoms that interfere with daily activities
Early evaluation can help guide appropriate treatment.
