Cervical Disc Herniation
Slipped Disc in the Neck
Quick Summary
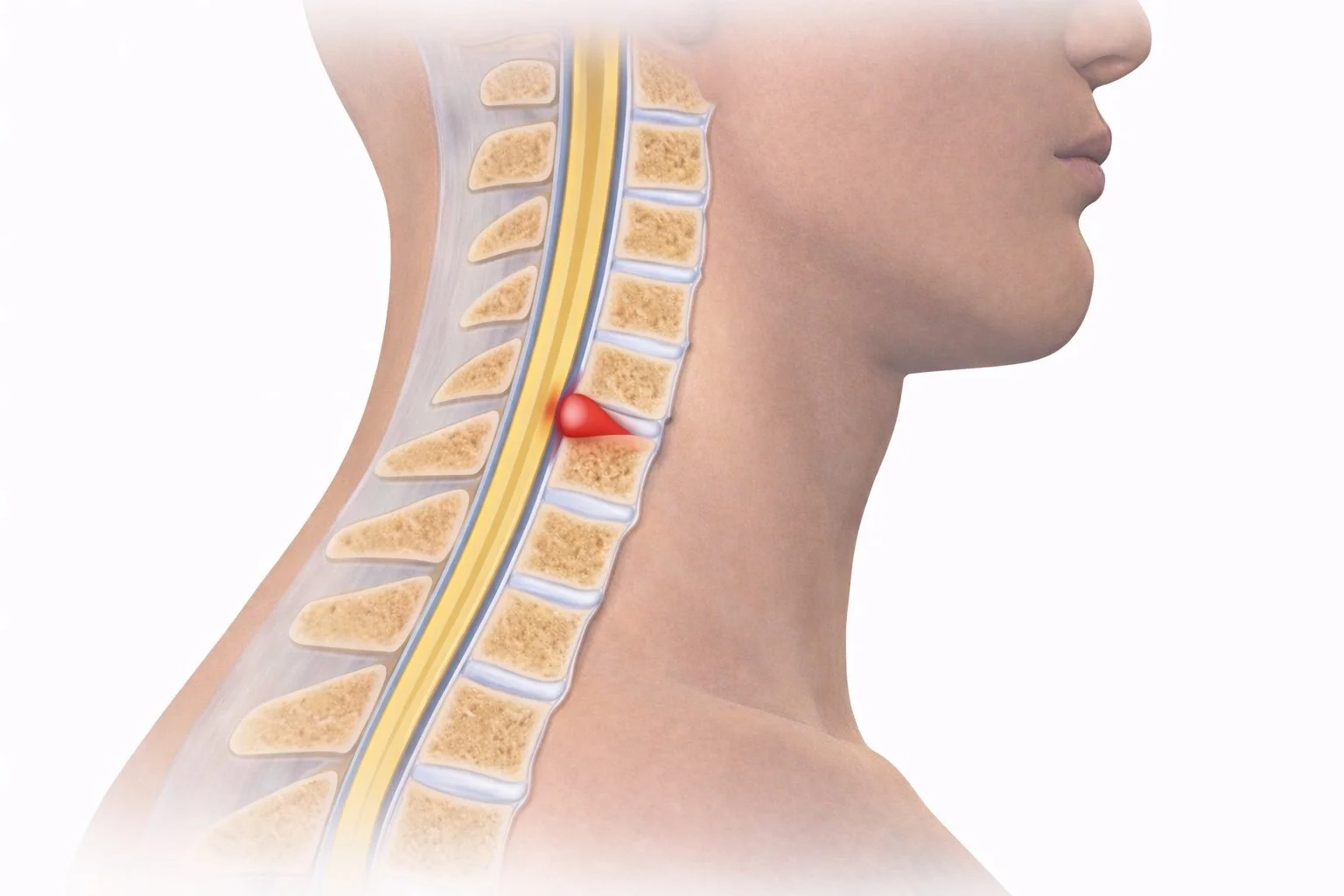
A cervical disc herniation (often called a slipped disc in the neck) occurs when a disc in the cervical spine is herniated outwards, which may pinch a nearby nerve.
Common cause of neck pain and arm pain
Often leads to cervical radiculopathy (pinched nerve)
Most patients improve without surgery
MRI is the best test to confirm the diagnosis
Surgery is considered only when symptoms do not improve or weakness develops
-
Cervical disc herniations most often occur in the lower neck, especially at C5–6 and C6–7, where motion and stress are greatest.
-
No. A disc herniation involves the disc itself, while arthritis affects the joints and bones. Many patients have some degree of both.
-
In many cases, symptoms improve over time as inflammation decreases and the body adapts.
What is a cervical disc herniation?
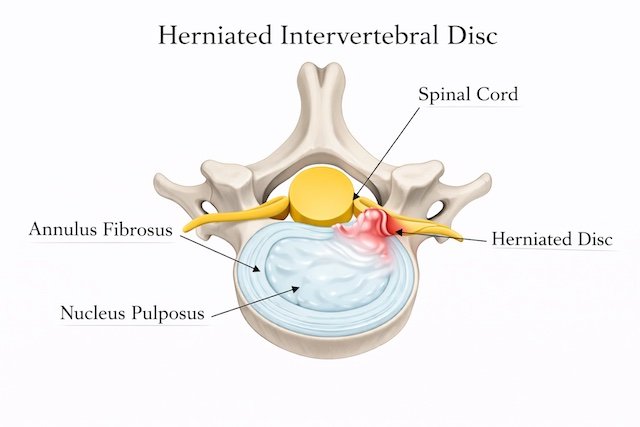
A cervical disc herniation happens when one of the discs in the neck bulges or ruptures and presses on a nerve or the spinal cord.
Discs sit between the bones of the spine and act as cushions. When the outer layer of a disc weakens, the soft center can push outward and cause symptoms.
Your cervical spine is your neck. Between the bones of your neck (vertebrae) are soft cushions called discs. These discs act like shock absorbers.
A cervical disc herniation happens when the soft center of a disc pushes out through its outer layer. When this happens, the disc can press on a nearby nerve or the spinal cord, which can cause pain or other symptoms.
What are the common symptoms of a cervical disc herniation?
Symptoms depend on which nerve is affected.
Common symptoms include:
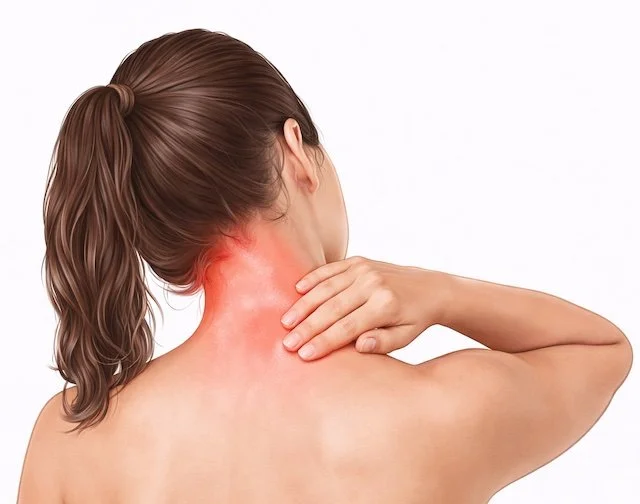
Neck pain
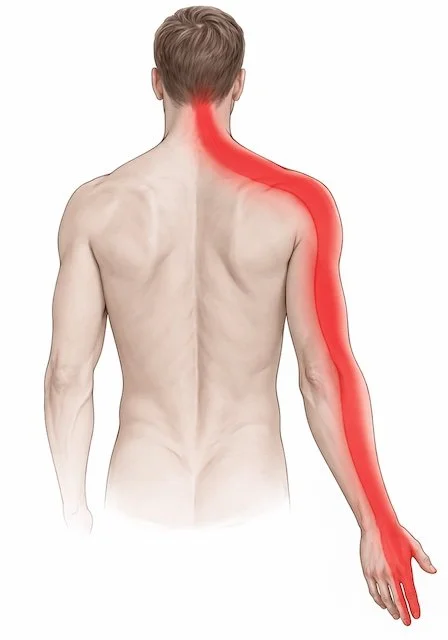
Pain that travels into the shoulder, arm, or hand
Numbness or tingling in the arm or fingers
Weakness in the arm or hand
Some people have a disc herniation on MRI but do not have symptoms.
-
Yes. Symptoms often fluctuate and may worsen with certain activities or positions.
-
Nerves exiting the neck travel down the arm. Pressure on these nerves can cause pain along their path.
-
Prolonged nerve compression can lead to lasting weakness, which is why worsening symptoms should be evaluated.
-
Progressive weakness, loss of coordination, or balance problems should be evaluated promptly.
What causes a cervical disc herniation?
Cervical disc herniations are most often caused by normal aging and wear over time.
Common causes include:
Wear and tear over time (degenerative changes)
Sudden injury, such as a fall or car accident
Repetitive strain or poor posture
Heavy lifting or twisting the neck
Many disc herniations happen without a clear injury and are part of the normal aging process.
-
Yes. Discs naturally lose water content over time, making them more prone to herniation.
-
Sudden movements or accidents can cause or worsen a disc herniation.
-
Repetitive neck strain or poor ergonomics may contribute to symptoms.
-
Some people are more prone to disc problems due to inherited factors.
How is a cervical disc herniation diagnosed?
Diagnosis begins with a detailed history and physical examination, focusing on strength, sensation, and reflexes. Imaging is often used to confirm the diagnosis and guide treatment.
An MRI is the most common imaging study, as it shows discs, nerves, and the spinal cord in detail.
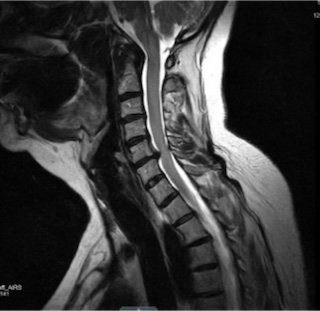
-
Not always. Many patients improve without imaging unless symptoms persist or worsen.
-
Yes. Imaging findings do not always correlate perfectly with symptoms.
-
Pain is influenced by inflammation, nerve sensitivity, and individual anatomy.
What are the non-surgical treatment options?
Non-surgical treatment is the first step for most patients and may include:
Activity modification
Anti-inflammatory medications
Physical therapy
Short courses of oral steroids or steroid injections
These treatments help reduce pain while the nerve heals.
-
Many patients improve within 6–12 weeks.
-
Injections reduce inflammation but do not remove the herniation.
-
Therapy is usually tailored to avoid worsening symptoms.
-
Some disc herniations improve over time, but persistent or worsening symptoms should be monitored.
When is surgery recommended?
Surgery may be recommended if:
Pain continues despite proper treatment
Weakness is present or worsening
Symptoms affect daily life or work
There is pressure on the spinal cord
The goal of surgery is to remove pressure from the nerve or spinal cord.
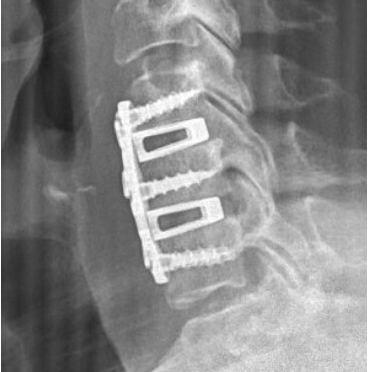
-
Most patients do not need surgery.
Many cervical disc herniations improve on their own over time. The body can slowly shrink the herniated disc and reduce nerve pressure.
-
Most cases are elective, but certain neurologic symptoms require prompt evaluation.
-
Early treatment can help prevent lasting deficits in appropriate cases.
-
Overall health and symptom severity are more important than age alone.
What types of surgery treat cervical disc herniation?
Common surgical options include:
Cervical disc replacement (for select patients)
Posterior Cervical Foraminotomy
Your surgeon will recommend the most appropriate option based on your condition.
-
Many patients return to light activity within weeks.
-
Most patients experience significant improvement in arm pain.
-
Recurrence is possible but uncommon.
-
Most patients return to work and exercise with guidance.

When should I see a spine specialist?
You should seek evaluation if you have:
Neck or arm pain persists despite treatment
You develop weakness, numbness, or coordination problems
Symptoms that interfere with daily activities
Early evaluation can help guide appropriate treatment.
