Lumbar Spinal Stenosis
Narrowing of the Spinal Canal in the Lower Back
Quick Summary
Lumbar spinal stenosis occurs when the spinal canal in the lower back becomes narrowed and places pressure on the nerves that travel into the legs.
Common cause of leg pain, numbness, or heaviness when walking
Symptoms often improve when sitting or leaning forward
Most often related to age‑related arthritis of the spine
MRI is the best test to diagnose the condition
Surgery may be recommended if symptoms significantly limit walking or daily activities
-
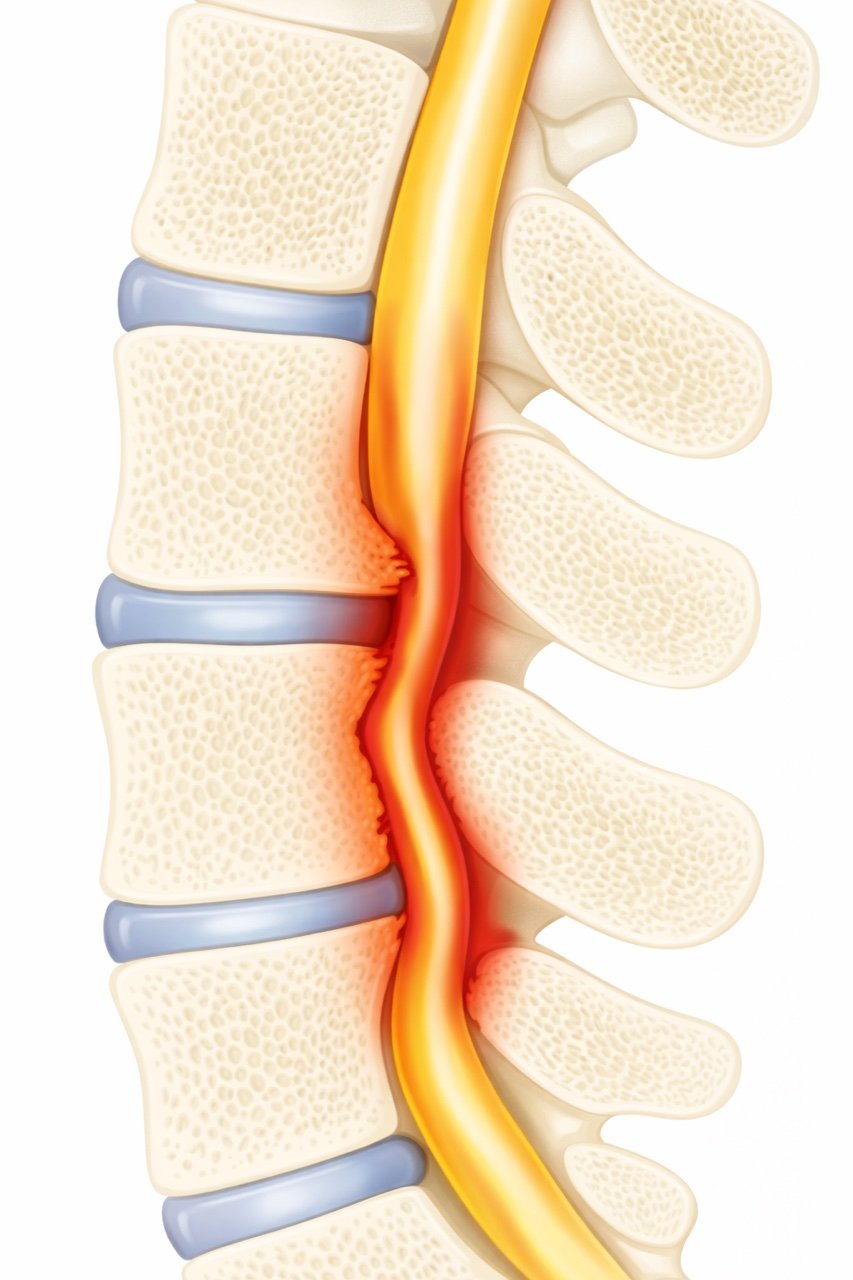
Stenosis simply means narrowing.
-
The nerves that travel from the lower back into the legs are affected.
-
Yes. Many patients have narrowing at several levels of the lumbar spine.
What is lumbar spinal stenosis?
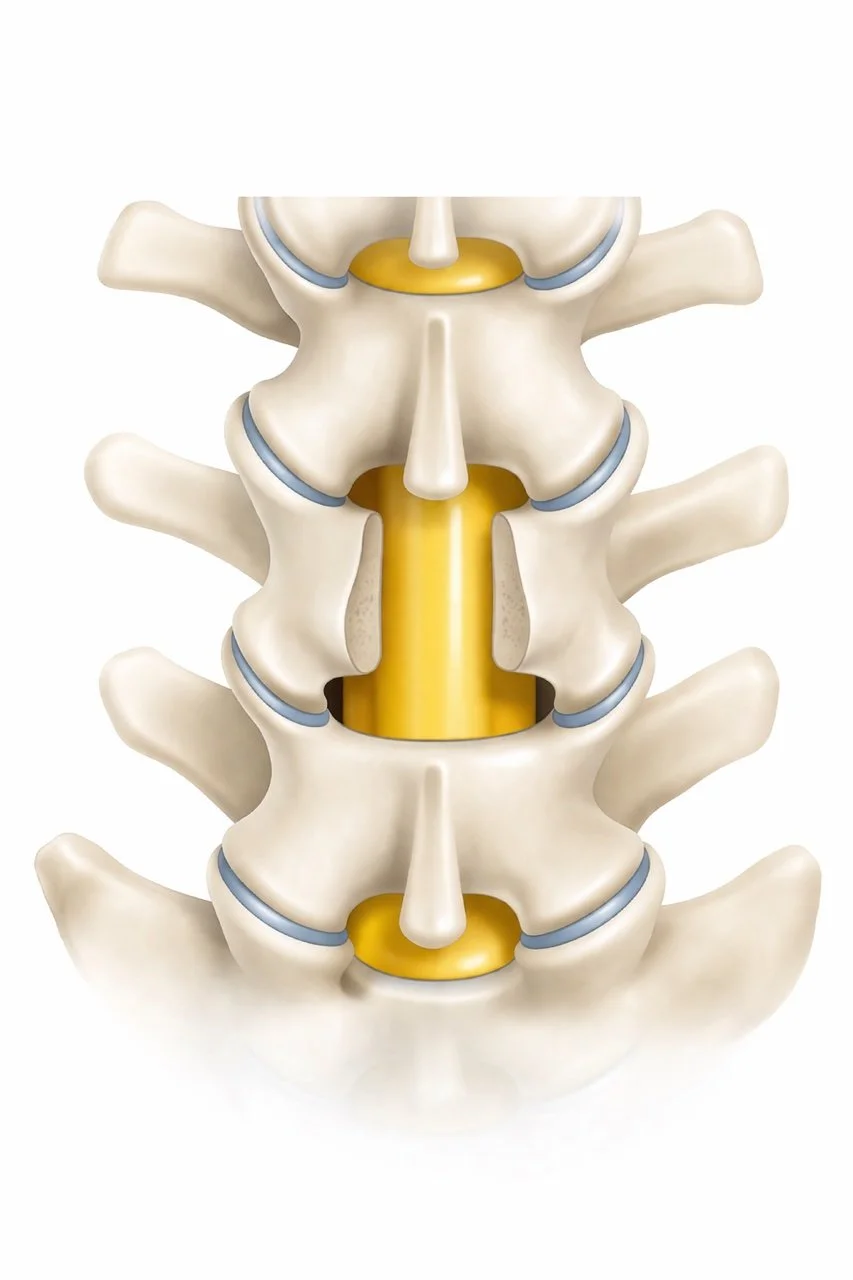
Lumbar spinal stenosis means that the space around the nerves in the lower back has become too narrow.
The spinal canal normally protects the nerves that travel from the spine into the legs. When this space narrows, the nerves can become compressed, leading to pain, numbness, or weakness in the legs.
What causes lumbar spinal stenosis?
The most common cause is age‑related arthritis of the spine.
Over time, several changes can narrow the spinal canal:
Thickened ligaments
Bone spurs from arthritis
Bulging or degenerating discs
Enlargement of joints in the spine
These changes gradually reduce the space available for the nerves.
-
Yes. It commonly develops as the spine ages.
-
Most cases develop gradually rather than from a single injury.
-
Yes. Some people are born with a narrower spinal canal.
What are the symptoms of lumbar spinal stenosis?
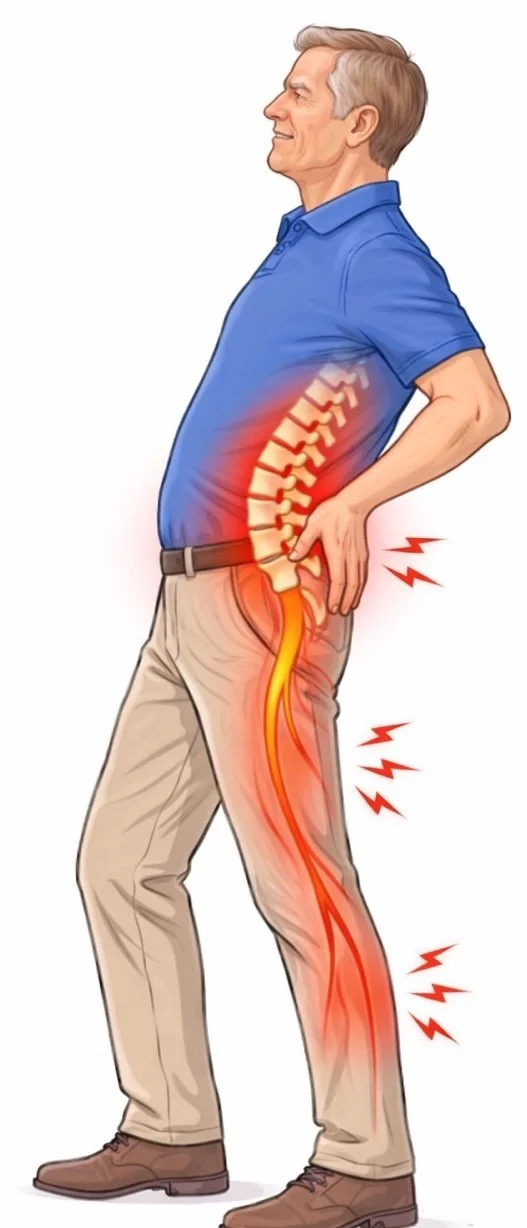
Symptoms usually involve the legs rather than the lower back.
Common symptoms include:
Pain, heaviness, or cramping in the legs
Numbness or tingling in the legs
Weakness with walking
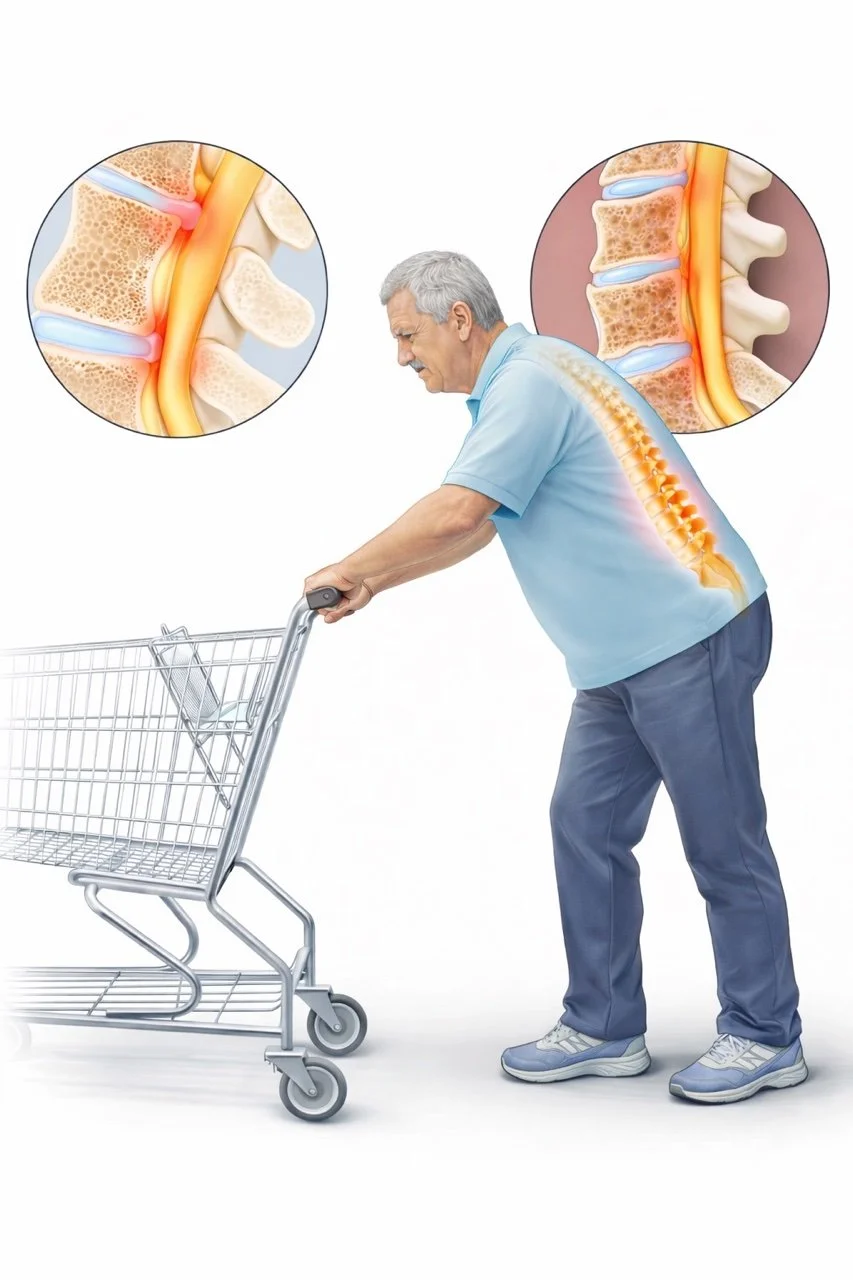
Symptoms that improve with sitting or bending forward
This pattern is sometimes called neurogenic claudication.
-
No. Other spine, nerve, or vascular conditions can also cause leg pain.
-
Pressure on the nerves reduces their ability to function normally during activity.
-
Sitting or bending forward increases space around the nerves.
-
Leaning forward opens the spinal canal slightly and relieves nerve pressure.
How is lumbar spinal stenosis diagnosed?
Diagnosis includes:
Review of symptoms
Physical and neurological examination
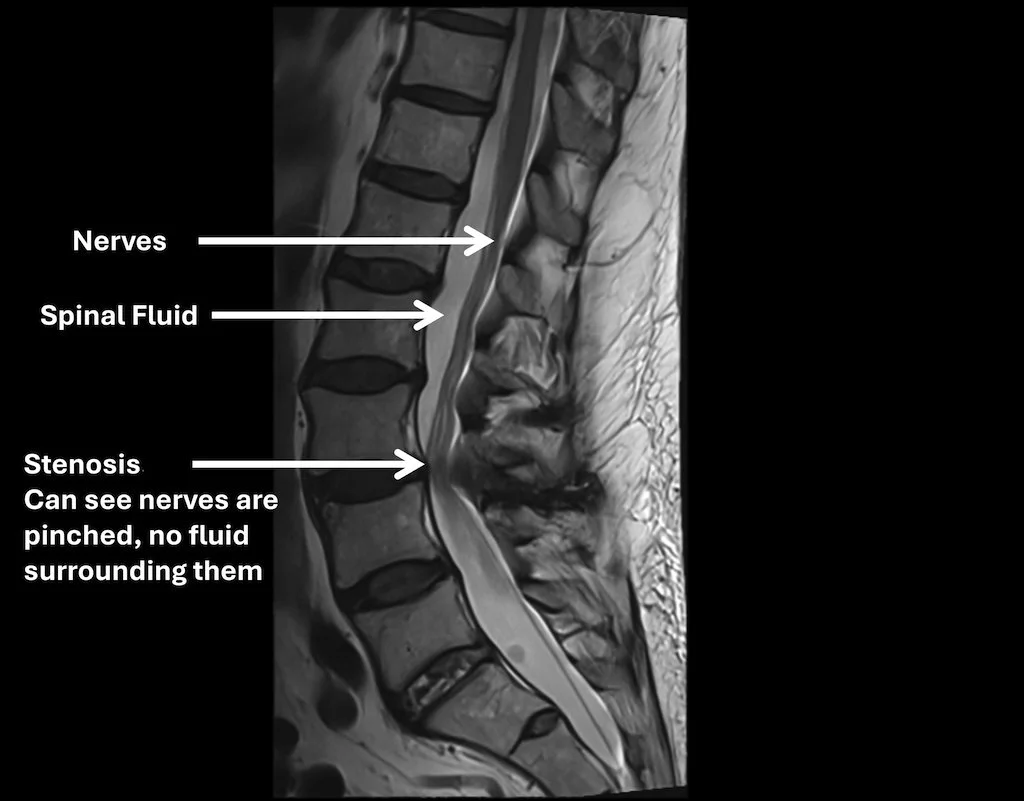
MRI of the lumbar spine
MRI shows the spinal canal, discs, joints, and nerves clearly and helps identify areas of narrowing.
-
MRI is helpful when symptoms persist or surgery is being considered.
-
X-rays show bones but not discs or nerves.
However, X-rays are also important because they can show your bone alignment and possibly other issues that are not shown on MRI.
-
Imaging must be interpreted together with your symptoms and exam.
Do I need surgery for lumbar spinal stenosis?
Many patients are treated without surgery.
Treatment depends on how much symptoms affect daily life and walking ability.
Surgery may be considered if:
Walking distance becomes very limited
Leg pain or numbness worsens
Non‑surgical treatments fail to provide relief
-
No. Many patients manage symptoms without surgery.
-
When symptoms significantly limit walking or quality of life.
-
It is rarely dangerous but can greatly affect mobility.
-
Surgery removes pressure from the nerve but does not stop aging of the spine.
What are the non-surgical treatment options?
Most patients begin with conservative treatment, which may include:
Physical therapy
Anti‑inflammatory medications
Activity modification
Epidural steroid injections
These treatments aim to reduce inflammation and improve function.
-
Therapy can improve mobility and reduce symptoms.
-
No. They reduce inflammation but do not reverse narrowing.
-
Walking is encouraged within a comfortable range.
What surgical options treat lumbar spinal stenosis?
Surgery focuses on creating more space for the nerves.
The most common procedure is a lumbar decompression (laminectomy), which removes bone and tissue that are compressing the nerves.
In some cases, spinal fusion may also be recommended if instability is present.
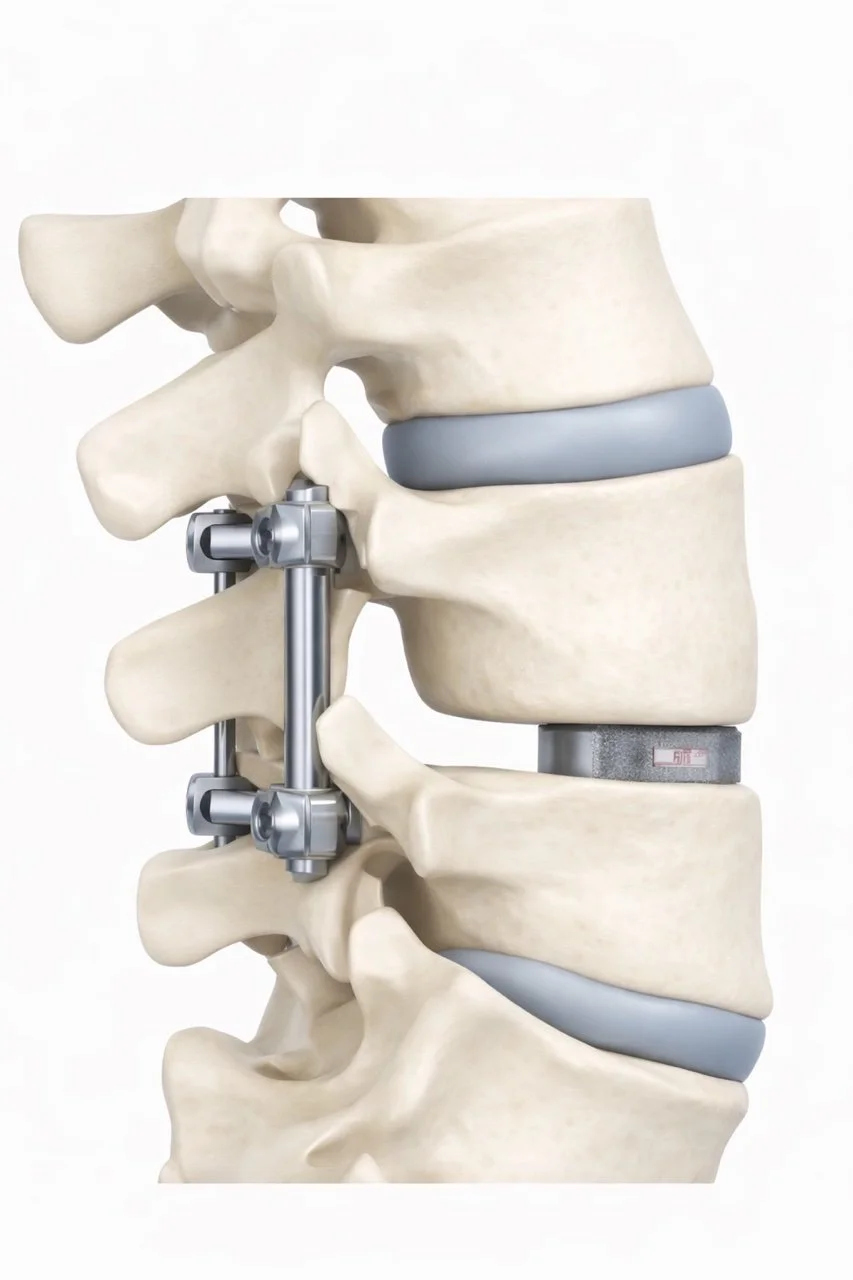
-
It is a procedure that removes bone and tissue to relieve pressure on the nerves.
-
Fusion is only needed if there is instability in the spine, or other factors such as severe arthritis or scoliosis.
-
Many decompression procedures can be performed using minimally invasive techniques.
What is recovery like after surgery?
Most patients experience improved walking and leg symptoms after decompression surgery.
Recovery typically involves gradual return to activity over several weeks.
-
Many patients notice improvement shortly after surgery.
-
Recovery varies but many patients return to normal activities within several weeks.
-
Some patients benefit from therapy to rebuild strength and mobility.


When should I see a spine specialist?
You should seek evaluation if you have:
Back pain lasting more than several weeks
Leg pain, numbness, or weakness
Symptoms that interfere with daily activities
Early evaluation can help guide appropriate treatment.
