Lumbar Radiculopathy
Pinched Nerve Causing Sciatica or Leg Pain
Quick Summary
Lumbar radiculopathy occurs when a nerve in the lower back becomes irritated or compressed. This condition often causes pain, numbness, or weakness that travels from the lower back into the leg.
Common cause of sciatica (pain traveling down the leg)
Symptoms usually affect one leg
Often caused by disc herniation or spinal stenosis
MRI is the best test to identify the cause
Most patients improve with non‑surgical treatment
-
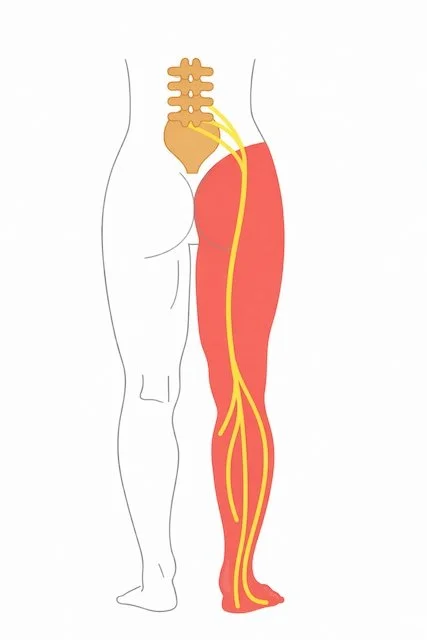
Radiculopathy means irritation or compression of a spinal nerve root.
-
Sciatica is the common term used when lumbar radiculopathy causes pain traveling down the leg.
-
It usually affects one leg, but in some conditions both legs may be involved.
What is lumbar radiculopathy?
Lumbar radiculopathy means that a nerve root in the lower spine is being compressed or irritated.
Each nerve leaving the lumbar spine travels into a specific part of the leg. When a nerve is pinched, pain, numbness, or weakness can occur along that nerve's pathway.
What causes lumbar radiculopathy?
Lumbar radiculopathy most commonly occurs when something presses on a spinal nerve.
Common causes include:
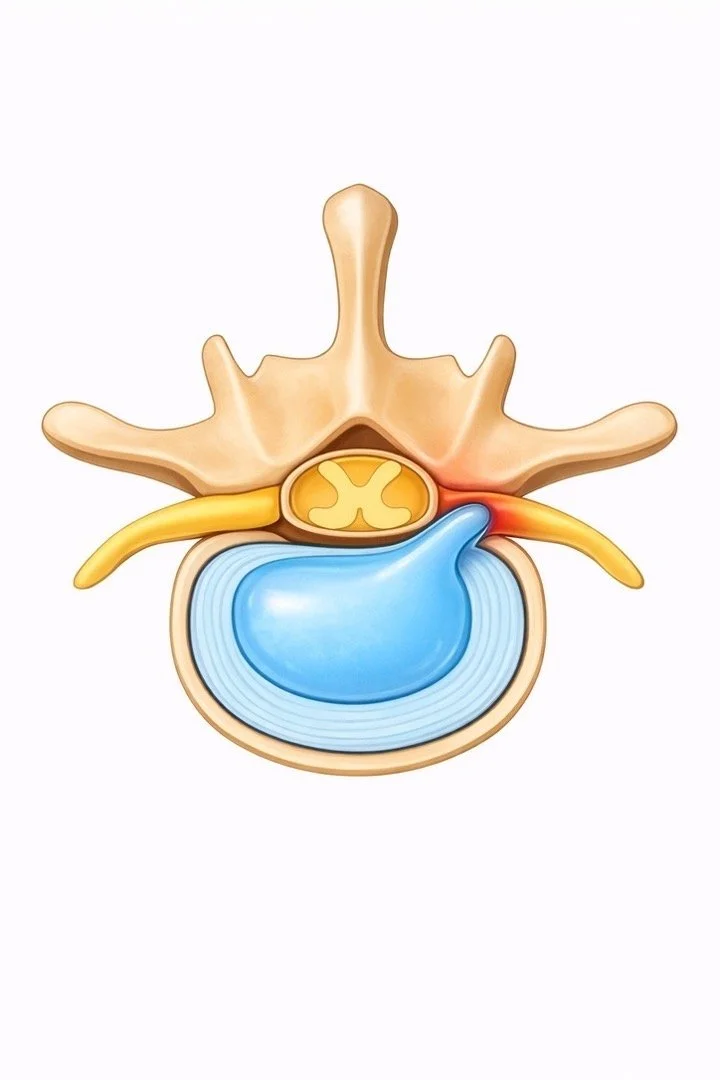
Lumbar disc herniation
Lumbar spinal stenosis
Bone spurs from arthritis
Narrowing of the nerve opening (foraminal stenosis)
These problems reduce the space around the nerve and lead to irritation.
-
A lumbar disc herniation is the most frequent cause.
-
Yes. Stenosis can narrow the space around nerves and compress them.
-
Yes. Many cases develop gradually due to degenerative changes.
What are the symptoms of lumbar radiculopathy?
Symptoms usually follow the path of the irritated nerve and may include:
Pain traveling from the lower back into the buttock or leg
Numbness or tingling in the leg or foot
Weakness in the leg or foot
Burning or electric‑like pain
Symptoms often worsen with certain movements or prolonged sitting.
-
The nerve irritation usually causes more leg pain than back pain.
-
The irritated nerve carries signals along its entire path into the leg.
-
Yes. Depending on the nerve involved, pain may extend to the foot.
How is lumbar radiculopathy diagnosed?
Diagnosis typically includes:
Discussion of symptoms
Physical and neurological examination
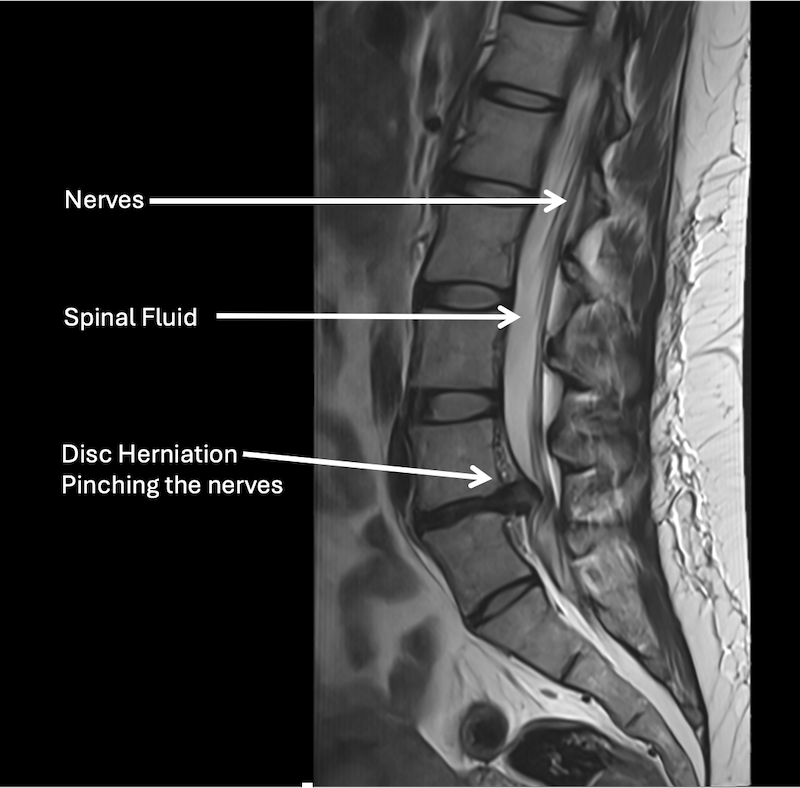
MRI of the lumbar spine when needed
MRI helps identify the structure that is compressing the nerve.
MRI helps identify disc herniation and nerve compression.
-
Not always. MRI is often recommended if symptoms persist or worsen.
-
X-rays show bones but not discs or nerves.
However, X-rays are also important because they can show your bone alignment and possibly other issues that are not shown on MRI.
-
Occasionally nerve studies may be used to confirm nerve irritation.
Do I need surgery for lumbar radiculopathy?
Most patients do not need surgery.
Many cases improve with time as inflammation decreases and the nerve recovers.
Surgery may be considered when:
Severe leg pain persists
Symptoms fail to improve after several weeks
Progressive weakness occurs
-
Yes. Many cases improve with time and conservative care.
-
Many patients try conservative care for at least 4-6 weeks, unless there is significant muscle weakness.
-
Urgent surgery is uncommon but may be needed if severe nerve problems occur.
-
Yes. Many nerves recover once inflammation improves.
What are the non-surgical treatment options?
Non‑surgical treatment often includes:
Activity modification
Anti‑inflammatory medications
Physical therapy
Epidural steroid injections
These treatments help reduce inflammation around the nerve.
-
Yes. Therapy can improve movement and reduce pressure on the nerve.
-
Injections help reduce inflammation but do not remove the underlying cause.
-
Gentle activity is usually better than prolonged bed rest.
What surgical options treat lumbar radiculopathy?
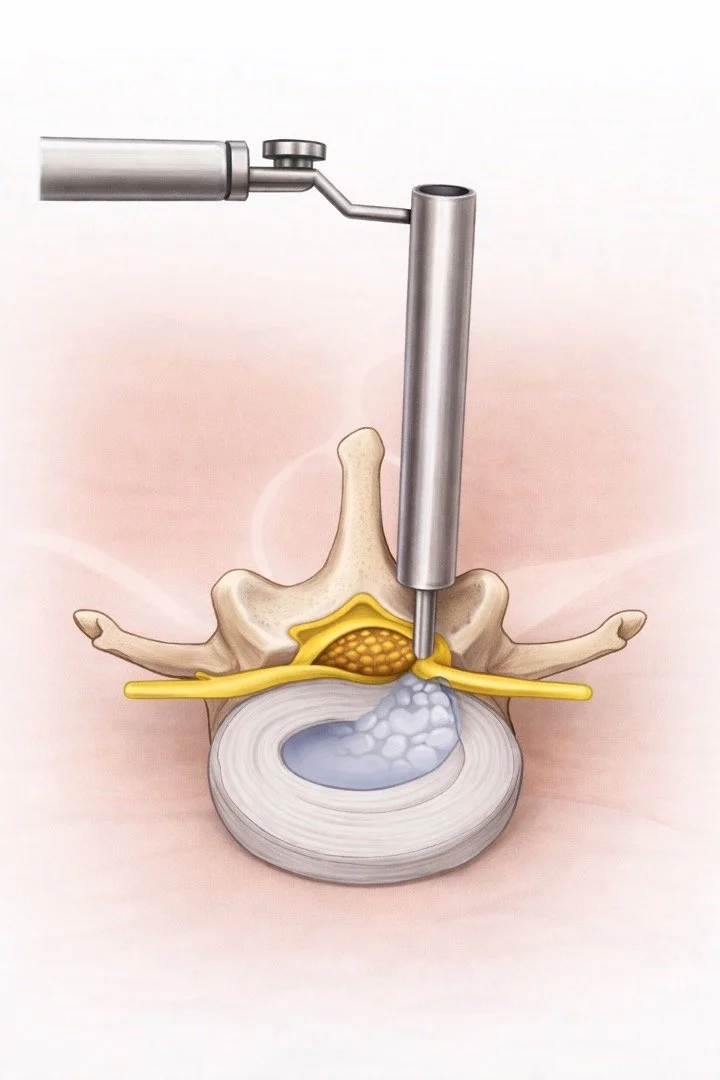
Surgery is aimed at removing pressure from the affected nerve.
The most common procedure is a lumbar microdiscectomy, which removes the portion of the disc pressing on the nerve.
In some cases, decompression surgery may also be used if stenosis is present.
-
It is a procedure that removes the portion of the disc compressing the nerve.
-
Many procedures use small incisions and specialized instruments.
-
Surgery is usually very effective at relieving leg pain.
What is recovery like after surgery?
Many patients notice rapid improvement in leg pain once pressure on the nerve is relieved.
Recovery involves gradually returning to normal activities over several weeks.
-
Many patients notice improvement soon after surgery.
-
Numbness may take longer to improve.
-
This depends on symptoms and the type of treatment performed.

When should I see a spine specialist?
You should seek evaluation if you have:
Back pain lasting more than several weeks
Leg pain, numbness, or weakness
Symptoms that interfere with daily activities
Early evaluation can help guide appropriate treatment.
