Lumbar Disc Herniation
Herniated Disc Causing Sciatica or Leg Pain
Quick Summary
Lumbar disc herniation occurs when a disc in the lower back bulges or ruptures and presses on a nearby nerve.
One of the most common causes of sciatica (leg pain)
Pain may travel from the lower back into the buttock, thigh, or foot
Often improves with non-surgical treatment
MRI is the best test to confirm the diagnosis
Surgery may be considered when pain or weakness does not improve
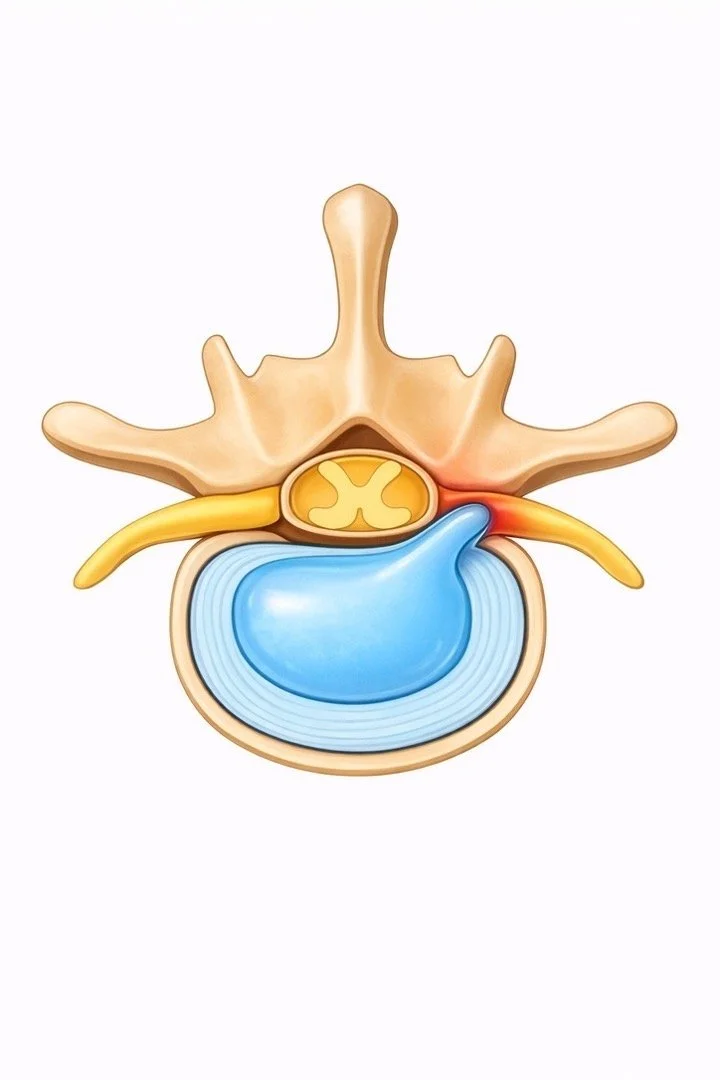
-
It means part of the disc has pushed outward and is pressing on a nerve.
-
Yes. "Slipped disc" is a common non-medical term for disc herniation.
-
Yes. Many herniated discs shrink over time as inflammation improves.
What is a lumbar disc herniation?
A lumbar disc herniation happens when the soft center of a spinal disc pushes through its outer layer and presses on a nearby nerve.
Discs sit between the bones of the spine and act like shock absorbers. When a disc herniates, it can irritate or compress the nerve that travels into the leg.
What are the symptoms of a lumbar disc herniation?
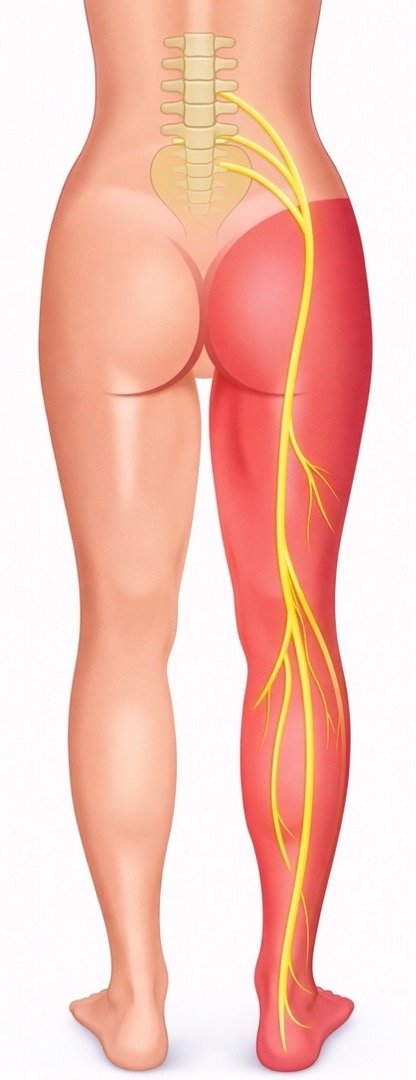
Symptoms often involve the lower back and one leg and may include:
Sharp or burning pain traveling down the leg
Numbness or tingling in the leg or foot
Weakness in the leg
Lower back pain
This pattern of leg pain is commonly called sciatica.
-
The nerve irritation usually causes more leg pain than back pain.
-
Sciatica refers to pain traveling along the sciatic nerve into the leg.
-
Yes. Depending on the nerve involved, pain may extend to the foot.
What causes a lumbar disc herniation?
Lumbar disc herniations can occur from disc degeneration, strain, or sudden injury.
Common contributing factors include:
Age-related disc wear
Heavy lifting or twisting
Repetitive bending
Sudden strain on the lower back
-
Often there is no single event. Disc herniations frequently occur gradually.
-
Heavy lifting or twisting can sometimes trigger symptoms.
-
The lumbar spine carries most of the body’s weight and stress.
How is a lumbar disc herniation diagnosed?
Diagnosis usually includes:
A detailed medical history
Physical and neurological examination
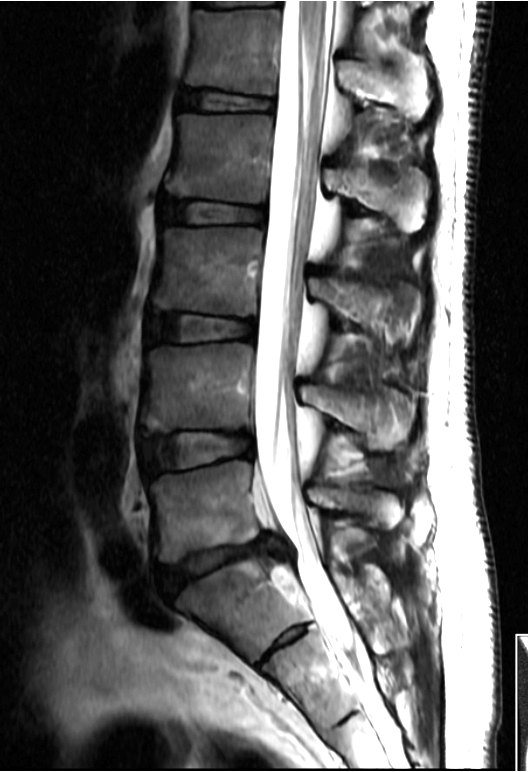
MRI of the lumbar spine
MRI helps identify disc herniation and nerve compression.
-
Not always. Imaging is usually done if symptoms persist or worsen.
-
X-rays show bones but not discs or nerves.
However, X-rays are also important because they can show your bone alignment and possibly other issues that are not shown on MRI.
-
Imaging helps guide diagnosis but must be interpreted with the physical exam.
Do I need surgery for a lumbar disc herniation?
Most patients do not need surgery.
Many disc herniations improve over several weeks as inflammation decreases and the nerve recovers.
Surgery may be considered if:
Leg pain remains severe
Symptoms persist despite treatment
Progressive weakness occurs
-
Yes. Many cases improve with time and conservative care.
-
Many patients try conservative care for at least 4-6 weeks, unless there is significant muscle weakness.
-
Urgent surgery is uncommon but may be needed if severe nerve problems occur.
-
Surgery removes pressure from the nerve but does not stop aging of the spine.
What are the non-surgical treatment options?
Most patients start with conservative treatment, which may include:
Activity modification
Anti-inflammatory medications
Physical therapy
Epidural steroid injections
These treatments aim to reduce inflammation around the nerve.
-
Yes. Therapy helps improve movement and reduce nerve irritation.
-
Injections reduce inflammation but do not remove the disc material.
-
Gentle activity is usually better than prolonged bed rest.
What surgical options treat lumbar disc herniation?
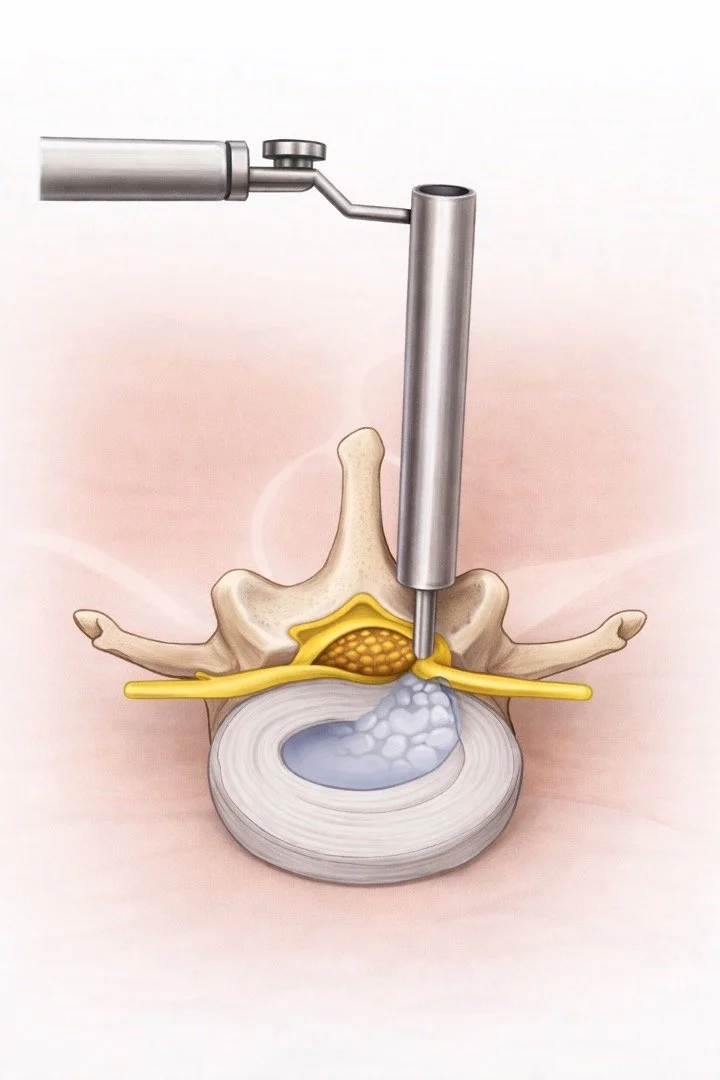
The most common surgery is a lumbar microdiscectomy, which removes the part of the disc pressing on the nerve.
The procedure is typically minimally invasive and focuses on relieving nerve pressure.
-
It is a procedure that removes the portion of the disc compressing the nerve.
-
Most procedures take about one hour.
-
Yes. Modern techniques use small incisions and specialized instruments.
What is recovery like after surgery?
Most patients experience rapid relief of leg pain after surgery.
Recovery usually includes gradual return to activity over several weeks.
-
Many patients notice improvement soon after surgery.
-
Numbness may take longer to improve.
-
Many patients resume light activities within a few weeks.

When should I see a spine specialist?
You should seek evaluation if you have:
Back pain lasting more than several weeks
Leg pain, numbness, or weakness
Symptoms that interfere with daily activities
Early evaluation can help guide appropriate treatment.
