Lumbar Spondylolisthesis
One Vertebra Slipping Over Another
Quick Summary
Lumbar spondylolisthesis occurs when one vertebra in the lower back slips forward over the bone below it.
Common cause of lower back pain and leg symptoms
Often associated with spinal stenosis or nerve compression
May develop from age-related degeneration or stress fractures
MRI and X‑rays help diagnose the condition
Many patients improve with non‑surgical treatment
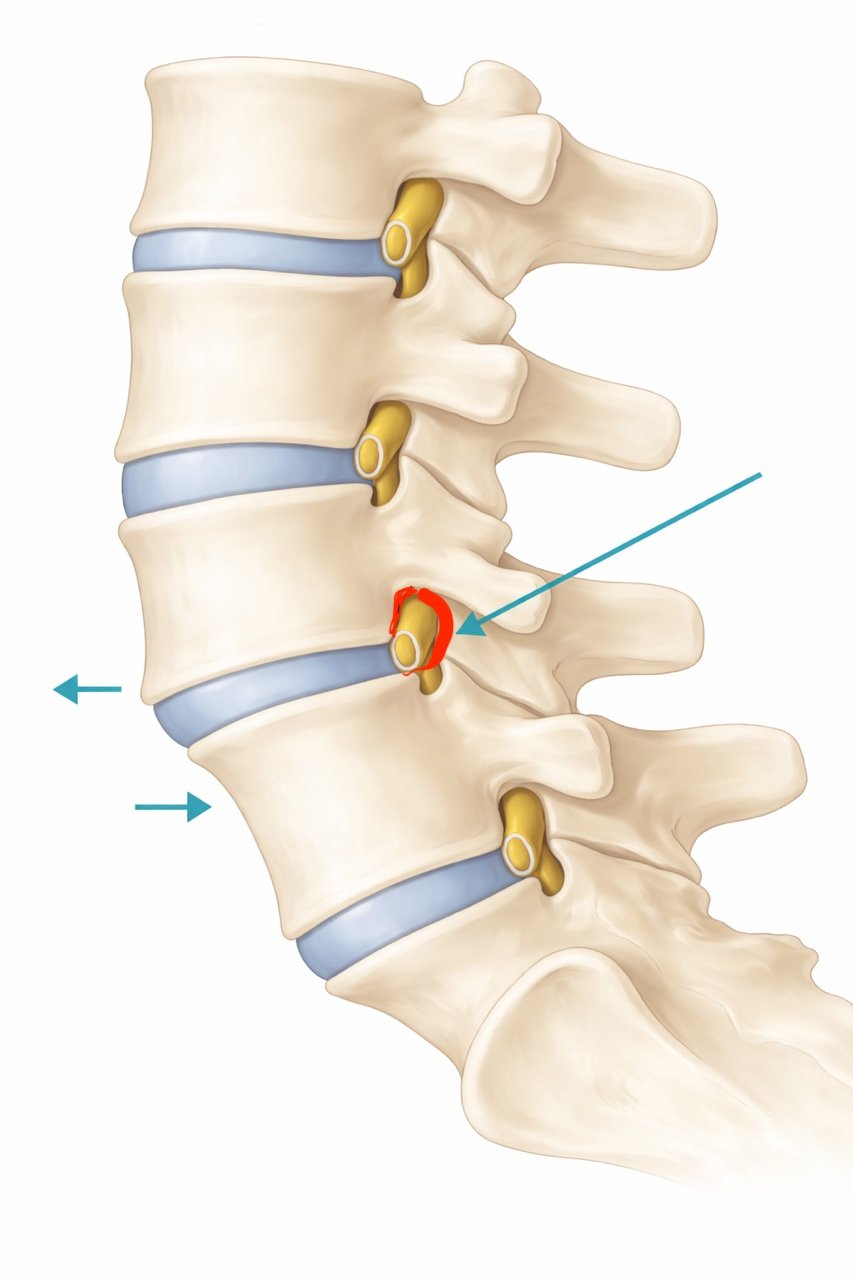
-
It means that one spinal bone has slipped forward relative to another.
-
Most cases are not dangerous, but the slip can irritate nearby nerves and cause symptoms.
-
Many slips remain stable, but some may progress slowly.
What is lumbar spondylolisthesis?
Lumbar spondylolisthesis means that one vertebra in the lower spine has shifted forward relative to the vertebra below it.
This shift can narrow the space for nearby nerves and sometimes create instability in the spine.
What causes lumbar spondylolisthesis?
There are several types of spondylolisthesis. The most common causes include:
Degenerative changes from aging and arthritis
Stress fractures in part of the vertebra (spondylolysis)
Congenital differences in spinal anatomy
Degenerative spondylolisthesis typically occurs in adults, while stress‑related slips may occur in younger patients.
-
It occurs when arthritis and disc wear allow one vertebra to shift forward.
-
Spondylolysis is a stress fracture in part of the vertebra that can lead to slippage.
-
Usually not. Most cases develop gradually over time.
What are the symptoms of spondylolisthesis?
Symptoms can vary depending on how much the nerves are affected.
Common symptoms include:
Lower back pain
Leg pain, numbness, or tingling
Weakness in the legs
Difficulty standing or walking for long periods
Many patients also have symptoms related to lumbar spinal stenosis.
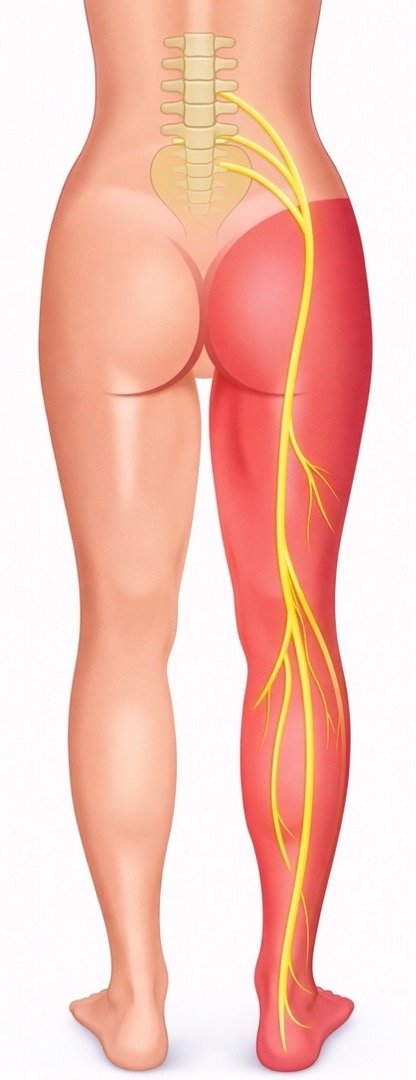
-
The slipped vertebra can narrow the space around nerves that travel to the legs.
-
Standing upright may increase pressure on the nerves.
-
Yes. Nerve compression from the slip can cause sciatica.
How is spondylolisthesis diagnosed?
Diagnosis typically includes:
Discussion of symptoms
Physical and neurological examination
X‑rays of the lumbar spine
MRI of the lumbar spine
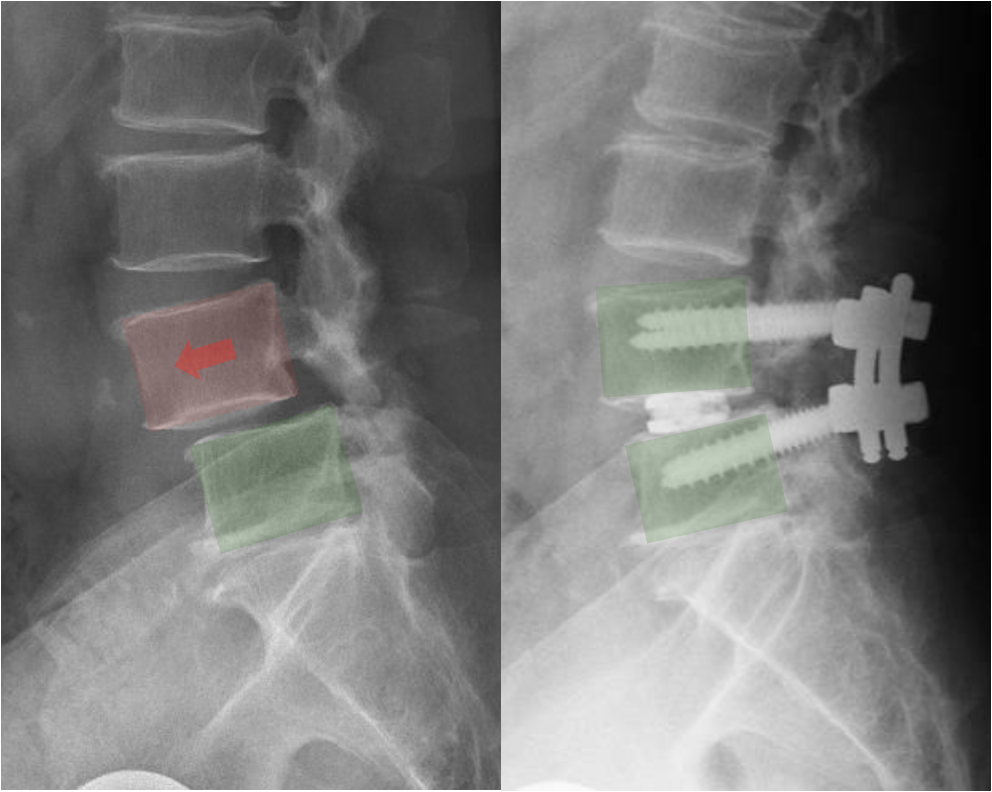
X‑rays show the amount of slippage, while MRI shows nerve compression.
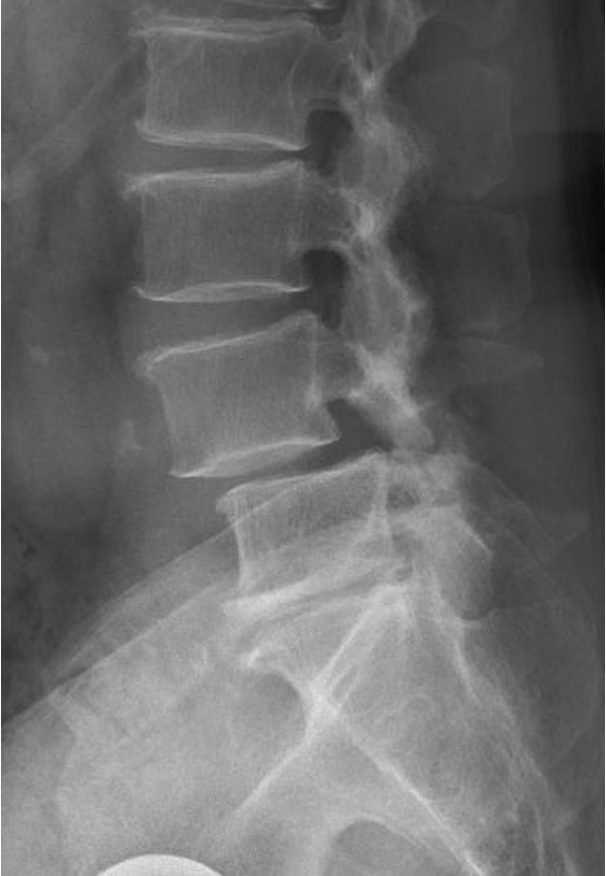
-
X‑rays clearly show how much one vertebra has shifted relative to another.
-
MRI shows nerves, discs, and areas of stenosis.
-
Symptoms and nerve compression are often more important than the exact amount of slip.
Do I need surgery for spondylolisthesis?
Many patients improve without surgery.
Treatment depends on symptoms, nerve compression, and stability of the spine.
Surgery may be considered when:
Leg symptoms significantly limit walking
Non‑surgical treatment fails
Nerve compression causes weakness
-
No. Many patients manage symptoms with conservative care.
-
Severe leg pain, nerve compression, or instability.
-
In most cases it is not urgent, but worsening nerve symptoms should be evaluated.
What are the non‑surgical treatment options?
Most patients begin with conservative treatment, which may include:
Physical therapy
Anti‑inflammatory medications
Activity modification
Epidural steroid injections
These treatments help reduce nerve irritation and improve stability.
-
Yes. Strengthening the core muscles helps support the spine.
-
No. Injections reduce inflammation around the nerves.
-
Gentle activity is usually encouraged within a comfortable range.

What surgical options treat spondylolisthesis?
When surgery is needed, the goal is to relieve nerve pressure and stabilize the spine.
Common procedures include:
Lumbar decompression (laminectomy)
Lumbar spinal fusion
Fusion helps prevent further movement between the vertebrae.
-
Fusion stabilizes the slipped vertebra and prevents further movement.
-
In select cases, decompression alone may be appropriate.
-
Surgery is generally effective at relieving leg symptoms and improving walking ability.
What is recovery like after surgery?
Recovery varies depending on the procedure performed.
Many patients notice improvement in leg pain soon after surgery and gradually return to activity over several weeks to months.
-
Initial recovery often takes several weeks, with continued healing over several months.
-
Many patients experience improvement, though recovery varies.
-
Therapy is often recommended to rebuild strength and mobility.

When should I see a spine specialist?
You should seek evaluation if you have:
Back pain lasting more than several weeks
Leg pain, numbness, or weakness
Symptoms that interfere with daily activities
Early evaluation can help guide appropriate treatment.
