Lumbar Degenerative Disc Disease
Age‑Related Disc Changes in the Lower Back
Quick Summary
Lumbar degenerative disc disease refers to age‑related changes in the discs of the lower back that can lead to back pain, stiffness, or sometimes leg symptoms.
Very common and often part of normal aging
Discs gradually lose height, hydration, and flexibility
Symptoms may include low back pain, stiffness, or occasional leg pain
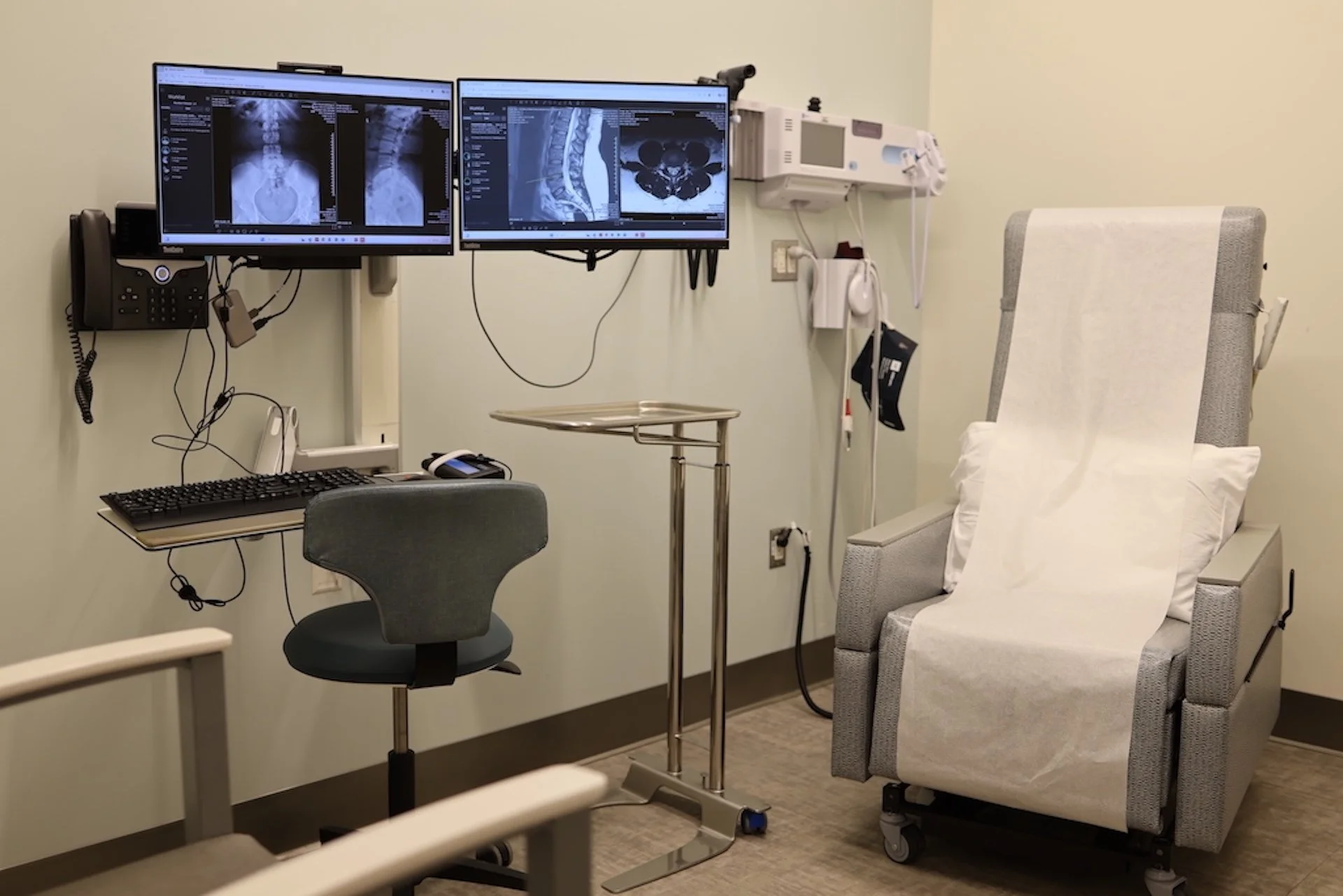
MRI helps evaluate disc health and related nerve pressure
Most patients improve with non‑surgical treatment
-
Not really. The term describes age‑related disc changes rather than a true disease.
-
Yes. Most people develop some degree of disc degeneration as they age.
-
Yes. Many people have disc degeneration on imaging but no symptoms.
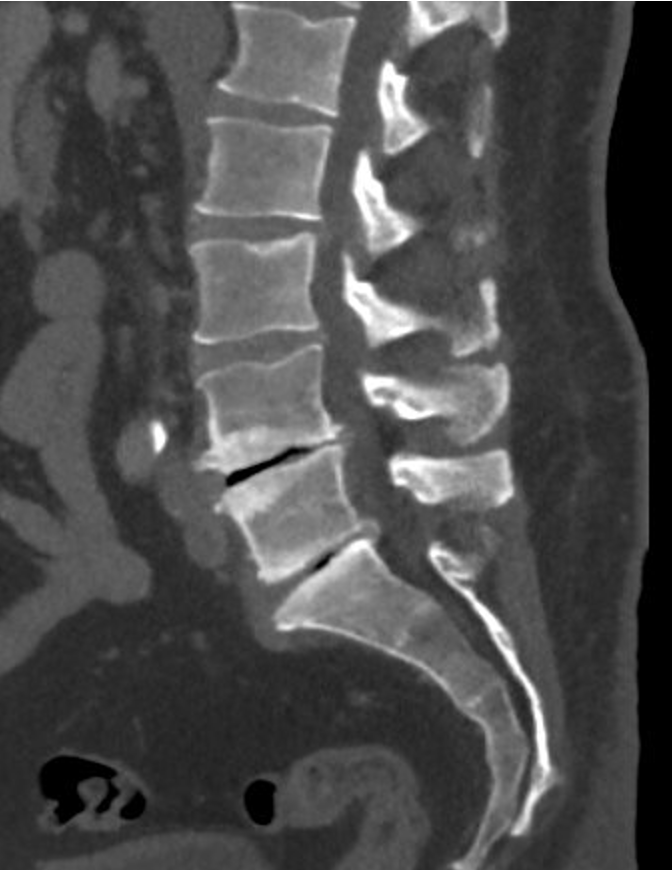
What is lumbar degenerative disc disease?
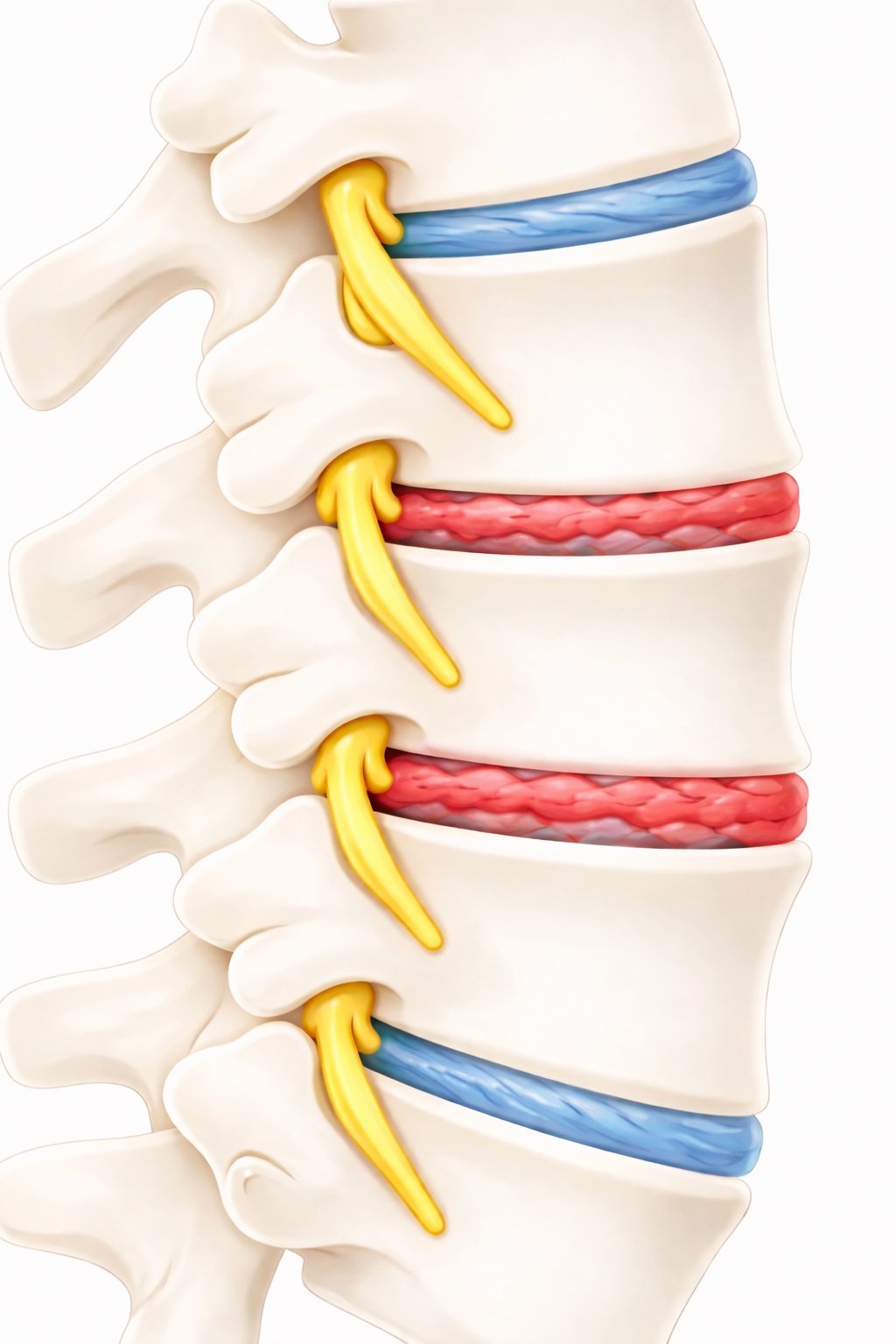
Lumbar degenerative disc disease describes the natural wear of the discs in the lower spine over time.
Spinal discs act as cushions between the bones of the spine. As they age, discs lose water content and elasticity. This can reduce their ability to absorb stress and may contribute to back pain or stiffness.
What causes lumbar degenerative disc disease?
The main cause is natural aging of the spine.
Other factors that may contribute include:
Genetics
Repetitive stress on the lower back
Prior injuries
Smoking
These factors can accelerate changes in the discs.
-
Usually no. Aging and genetics are the most important factors.
-
Heavy strain can trigger symptoms but usually does not cause degeneration alone.
-
It cannot be completely prevented, but healthy habits help support spine health.
What are the symptoms of lumbar degenerative disc disease?
Symptoms may vary and often involve the lower back.
Common symptoms include:
Aching pain in the lower back
Stiffness, especially after rest
Pain that worsens with prolonged sitting
Occasional pain traveling into the buttock or leg
Symptoms may fluctuate over time.
-
Degenerated discs move less smoothly and can lead to stiffness after rest.
-
Sitting increases pressure on the discs in the lower back.
-
Yes, if nearby nerves become irritated.
How is lumbar degenerative disc disease diagnosed?
Diagnosis usually includes:
Discussion of symptoms
Physical examination
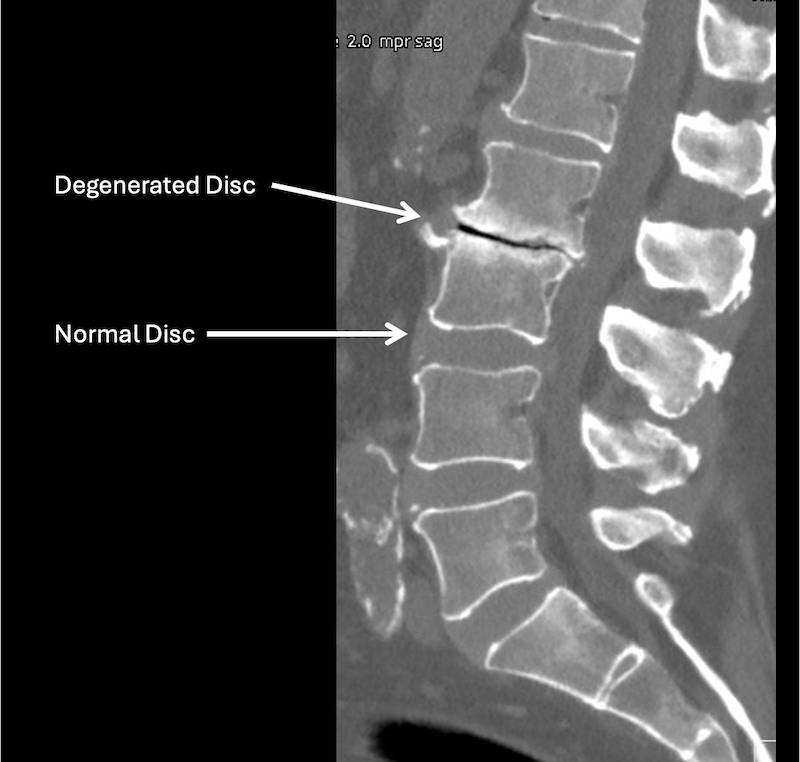
MRI of the lumbar spine when symptoms persist
MRI can show disc dehydration, loss of disc height, and related changes.
-
Not always. MRI is usually recommended when symptoms persist or worsen.
-
X‑rays can show certain changes such as disc height loss, and bone spur formation. They do not show nerves.
However, X-rays are also important because they can show your bone alignment and possibly other issues that are not shown on MRI.
-
Not always. Imaging findings and symptoms do not always match.
How is lumbar degenerative disc disease treated?
Most patients improve with non‑surgical treatment.
Treatment options may include:
Physical therapy
Anti‑inflammatory medications
Activity modification
Core strengthening exercises
These treatments aim to reduce pain and improve spine support.
-
Yes. Strengthening the core muscles helps support the spine.
-
Gentle activity is usually better than complete rest.
-
Injections may reduce inflammation but do not reverse degeneration.

Do I need surgery for lumbar degenerative disc disease?
Most patients do not require surgery.
Surgery may be considered if:
Severe back pain persists despite treatment
Symptoms significantly limit daily activities
Nerve compression causes leg symptoms
-
Because many people have degeneration without symptoms.
-
Severe persistent back pain or nerve compression symptoms.
-
No. Surgery treats symptoms but does not stop aging changes.
What surgical options are used if needed?
When surgery is appropriate, options may include:
Lumbar spinal fusion
Lumbar disc replacement (in select patients)
The goal of surgery is to stabilize the painful segment or relieve nerve pressure.
-
Fusion joins two vertebrae together to eliminate painful motion.
-
Yes, but only for certain patients.
-
Your surgeon considers symptoms, imaging, and overall spine alignment.
What is the long‑term outlook?
Many patients manage symptoms successfully with conservative care.
Disc degeneration often stabilizes over time and does not always worsen.
-
Not necessarily. Many patients improve over time.
-
Yes. Regular movement helps maintain spine health.
-
The disc will not regenerate, but symptoms can improve.

When should I see a spine specialist?
You should seek evaluation if you have:
Back pain lasting more than several weeks
Leg pain, numbness, or weakness
Symptoms that interfere with daily activities
Early evaluation can help guide appropriate treatment.
